Big gains and limitations: Reviewing my Fabry disease symptoms
A columnist gives himself a mental checkup on his decades with the condition
Written by |

I’ve been receiving biweekly infusions of enzyme replacement therapy for Fabry disease for over 20 years, and I had a heart transplant in September 2020. With these two amazing gifts, almost all my Fabry symptoms have improved significantly.
Those gains are multifarious and have bettered my quality of life, though I still endure some limitations. Today, as I give myself a mental checkup of sorts, I’m overall pleased.
Among my gains, my Fabry-related chronic kidney disease (CKD) has improved from stage 3 to stage 2 (stage 5 is near or at kidney failure) over my 20 years with the condition. My lung function has also improved, from below 50% at its lowest point to within the range of normal function.
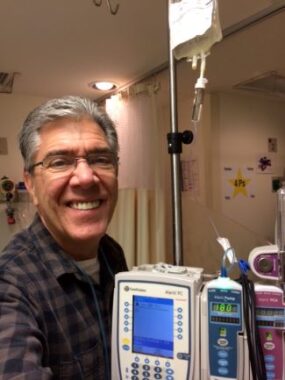
Jerry gets an infusion in 2014. (Courtesy of Jerry Walter)
Chronic gastrointestinal issues that disrupted my life for over 25 years are barely noticeable today, making the location of the next bathroom no longer an essential travel consideration. Chronic pitting lymphedema, which made my lower legs and ankles uncomfortable, rarely occurs anymore. When it does, it’s easily managed with compression socks and adequate sleep.
The apprehension I’ve felt for 30 years about premature death from Fabry is a much lighter burden now. My life has changed for the better!
While I’ve had many health improvements and added years of life, I’ve also faced some limitations of my treatment. I have severe hearing loss in my right ear, for instance, and profound loss in my left. I can’t communicate without my hearing aids and a special desk phone with a volume-boost feature. My hearing isn’t expected to improve.
Further, firsthand examples frequently remind me of another common manifestation of Fabry: neuropathic pain. I often experience sudden sharp or stinging pains in my legs, feet, arms, and hands, caused by the small-fiber neuropathy common with Fabry.
I’m not alone. Most people with Fabry report various levels of pain, ranging from mild to debilitating. Neuropathic pain as well as chronic gastrointestinal issues, such as abdominal pain and symptoms akin to irritable bowel syndrome, have an adverse impact on a Fabry patient’s quality of life.
My sporadic pains, however, usually subside quickly, so I flinch and grimace, then keep calm and carry on, as the popular meme says.
Some forms of Fabry pain, as described in a 2021 article in the journal Pain, are “burning, searing, squeezing, pressing, dragging, prickling, electrifying, tingling, sharp, and sore.” Heat, according to the article, is the most common pain trigger for Fabry patients. I rarely have burning pain except when I have a fever.
For much of my life, though, I’ve experienced periods of chronic, mild to severe flulike aches. They affect my entire body when triggered by hot or cold temperatures, temperature changes, fevers, stress, physical exertion, or sometimes for no apparent reason. The aches aren’t as easily dismissed as the frequently sharp but brief stinging pains.
When the overall achiness is severe, I need bed rest for a day or two. I think others refer to this as a pain crisis. To ease the pain, I use Tylenol (acetaminophen) first to take the edge off enough to push through my activities. I’ve always tried to refrain from taking ibuprofen because it’s harder on our kidneys than acetaminophen.
Some people with Fabry say Tylenol doesn’t help them with their pain, so they go right to stronger medications. Those tend to make my mind fuzzy, and I need a clear mind to do my work.
Chronic overall achiness limited or prevented my participation in many activities over the years. During my childhood, I was the kid who left the baseball field halfway through the game with my head down because I wasn’t tough enough. Later, the pain sometimes affected my work. I’d try to avoid circumstances that caused it — or I just pushed through it, if possible.
During my 27-year active-duty military career, I was somewhat of a physical underachiever, compared with other soldiers, because of Fabry-induced pain, hypohidrosis (reduced sweating), and overheating easily. But I was determined to always be good at my job and passed the required periodic physical fitness tests. Thanks to brains over brawn, a lot of Tylenol, and more office positions than field positions, I was able to have a great military career.
My life with Fabry disease is one among many unique experiences and journeys with this condition. My quality of life and experiences have been good to great, despite a few bumps on this road less traveled. I’ve had a lot of big gains! And I have a new life. The pain I still experience is small in comparison.
Note: Fabry Disease News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Fabry Disease News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to Fabry disease.







Leave a comment
Fill in the required fields to post. Your email address will not be published.